Overview
Spirometry is the most important pulmonary function test that measures lung function, specifically the amount (volume) and/or speed (flow) of air that can be inhaled and exhaled. It is a noninvasive procedure used for diagnosing and assessing conditions such as asthma, COPD, pulmonary fibrosis and cystic fibrosis.
Spirometry is considered as the primary examination for asthma diagnosis. It should be performed prior to starting treatment in order to establish the presence and determine the severity of baseline airway obstruction.
Monitoring asthma with a spirometry test is helpful, because you may not always be able to tell, just from your symptoms, whether or not your asthma is under control.
Recommendations for Spirometry
Children older than age five, and adults of any age, who have asthma-like symptoms should have a spirometry test. The NHLBI guidelines recommend that all persons with asthma have spirometry done at the beginning of care, again as treatments are started, and at least every one to two years for ongoing care.
Preparation for Spirometry
Wear comfortable, loose clothing. You shouldn’t smoke one hour before a spirometry test. You’ll also need to avoid alcohol that day as well. Exercising vigorously or eating a large meal before the test also impacts your ability to breathe. Your doctor may also have instructions about whether you should avoid using inhaled breathing medications or other medications prior to your test.
Spirometry Procedure
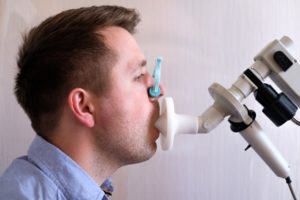
Your doctor will give you a mouthpiece connected to a spirometer or a laptop. They will have you take a deep breath and blow air out of your lungs as fast and as hard as you can. You may be asked to repeat the test a few times to get a valid test. The attempt does not count if you cough, if there is a delay in exhaling, or if you stop breathing too early.
If the results show reduced lung function, your doctor may give you a medication that opens your airways, called a bronchodilator. Fifteen to 30 minutes after taking the medication, you will be asked to do spirometry again to see if your lung function improves. This helps them make the correct diagnosis.
Spirometry Results
There are three main results from spirometry:
- Forced Expiratory Volume (FEV) – The amount of air you can forcefully exhale in one second.
- Forced Vital Capacity (FVC) – The maximum amount of air you can forcefully exhale.
- FEV/FVC – The percentage of your total air capacity that you can forcefully exhale in one second.
To Diagnose asthma, having a low FEV and low FEV/FVC means that the air has a hard time leaving the lungs, which indicates airway obstruction. The results after taking bronchodilator help separate asthma from COPD. If FEV increases by 12% or 200 mL after taking bronchodilator, it means that the airway blockage is reversible. Reversibility is a sign of asthma.
Spirometry is repeated after you have started taking medications to see how well medications are working.
Words like mild, moderate, or severe may be used to describe how severe the problem is. Ask your doctor to explain the results so that you know what they mean for you.
Bottomline
Spirometry is a valuable advancement in medical practice which helps physicians to accurately assess the condition of the patient’s lungs.
Whether you’ve already been diagnosed with a breathing problem or you think you may have one, ask your doctor about having a spirometry test soon.
Dr. Amy Schiffman, an asthma specialist, uses a computerized spirometer to effectively monitor the lung function of asthmatic patients. Schedule your appointment today!